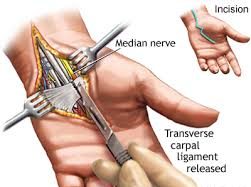
Carpal tunnel syndrome
A brain tumour is a mass of abnormally growing cells in the brain or skull. Half of the time it will have spread from somewhere else in the body (metastatic brain tumour). But sometimes it can just start from the brain (primary tumour) the tumours are named from the tissue type where they originate from